Reading Ekgs Life in the Fast Lane
ECG (EKG) Estimation
Equally with all investigations the near important things are your findings on history, examination and basic observations. Having a good arrangement will avoid making errors.
To commencement with we will comprehend the nuts of the ECG, how information technology is recorded and the basic physiology. The 12-lead ECG misleadingly only has 10 electrodes (sometimes also called leads but to avert confusion we will refer to them as electrodes).
The leads can exist idea of as taking a picture of the heart'south electric action from 12 different positions using information picked up past the 10 electrodes. These comprise 4 limb electrodes and half-dozen chest electrodes.
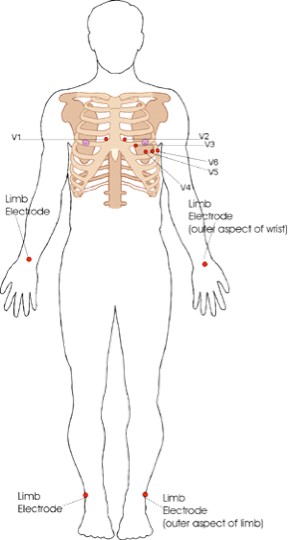
Figure 1. Electrode positions on an ECG (EKG).
When electric activity (or depolarisation) travels towards a pb, the deflection is net positive. When the action travels away from the pb the deflection is cyberspace negative. If information technology is at ninety degrees and then the complex is 'isoelectric' i.e. the R and South wave are the same size. This can often be seen in V4 (meet Figure 3).
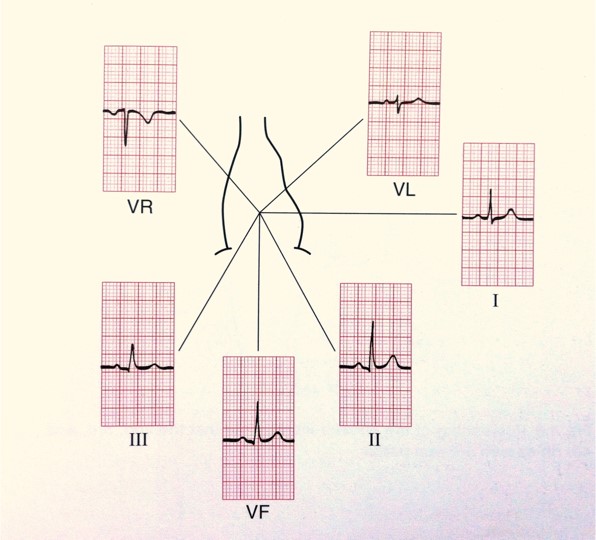
Figure 2. The electrical activity on an ECG (EKG).
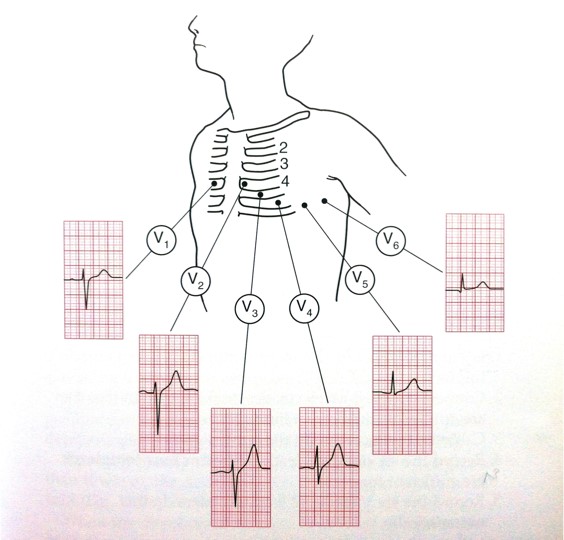
Figure 3. The electrical activity on an ECG (EKG).
The areas represented on the ECG are summarized beneath:
- V1, V2 = RV
- V3, V4 = septum
- V5, V6 = L side of the heart
- Pb I = 50 side of the heart
- Atomic number 82 II = inferior territory
- Pb III = inferior territory
- aVF = junior territory (call back 'F' for 'anxiety')
- aVL = 50 side of the heart
- aVR = R side of the center
The ECG can exist broken downward into the individual components. For the purpose of this we will look at lead Two (see Figure 4). All boxes are based on the supposition that the paper speed is running at 25mm/sec, therefore ane large square is equivalent to 0.2 secs and a small square to 0.04 secs.
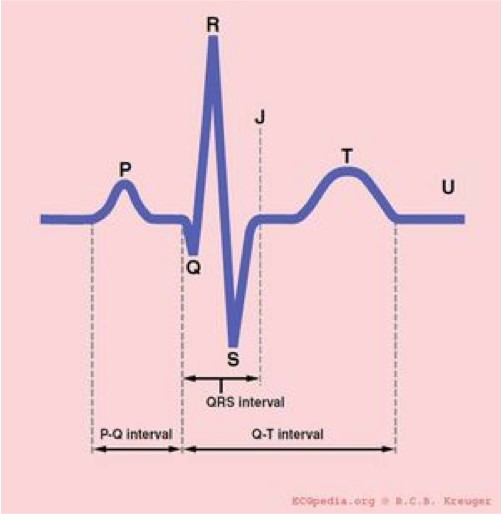
Effigy 4. The segments of the ECG.
What practice the segments of the ECG represent?
- P-moving ridge: Atrial wrinkle
- PR interval: Represents the fourth dimension taken for excitation to spread from the sino-atrial (SA) node across the atrium and downwards to the ventricular muscle via the packet of His.
- QRS: Ventricular contraction
- ST segment: Ventricular relaxation
- T-wave: Ventricular repolarisation
Normal duration of ECG segments:
- PR interval: 0.12 – 0.ii secs (three-five small squares)
- QRS: <0.12 secs (3 small squares)
- QTc: 0.38 – 0.42 secs
How to read an ECG
At that place are many different systems to translate the ECG. This system ensures y'all will never miss anything:
- Patient details
- Situation details
- Charge per unit
- Rhthm
- Axis
- P-wave and P-R interval
- Q-wave and QRS complex
- ST segment
- QT interval
- T-wave
These components volition at present exist explained in more particular.
1. Patient details
- Patient'southward proper noun, date of nascence and hospital number
- Location
- This becomes important as in the ED or acute medical setting doctors are oft shown multiple ECGs. You demand to know where your patient is in club to ensure that they tin can exist moved to a higher dependency area if advisable.
2. Situation details
- When was the ECG done?
- The fourth dimension
- The number of the ECG if information technology is one of a series
- If you lot are concerned that there are dynamic changes in an ECG it is helpful to ask for serial ECGs (usually three ECGs recorded 10 minutes apart) and then they can be compared. These should ever be labelled one, 2 and 3.
- Did the patient accept chest pain at the time?
- Or other relevant clinical details. For example, if you are wanted an ECG to expect for changes of hyperkalaemia, annotation the patient's potassium level on the ECG.
3. Measuring the rate on an ECG
- Rate can be calculated in a number of means:
- Count the number of QRSs on ane line of the ECG (usually atomic number 82 Two – running along the bottom) and multiply by half-dozen.
- Count the number of large squares betwixt R waves and divide 300 by this number (if the patient is in atrial fibrillation it is more than accurate to report a rate range rather than a single value).
4. Assessing the rhythm on an ECG
- Is the rhythm regular or irregular? If information technology is irregular is it regularly or irregularly irregular?
- Rhythm can exist difficult to appraise especially in bradycardia or tachycardia. It may be helpful to utilise the 'paper exam'.
- To practice this place a piece of flake paper over the ECG and mark a dot next to the top of a QRS complex, describe some other dot adjacent to the pinnacle of the next QRS so slide the paper along the ECG. If the rhythm is regular you should see that your 2 dots match to the tops of the QRS complexes throughout the ECG.
5. Assessing the axis on an ECG
- Axis is the sum of all the electrical activity in the middle.
- The contraction travels from the atria to the correct and left ventricles. As the left ventricle is larger and more muscular normal axis lies to the left (at -30 degrees to ninety degrees – meet Figure 5).
- As a general rule if the cyberspace deflections in leads I and aVF are positive and then the axis is normal.
- If lead I has a net negative deflection whilst aVF is positive and so at that place is right centrality deviation.
- If lead I has a positive deflection and aVF has a negative deflection and so there is left axis deviation
- If you want to piece of work it out more precisely you can apply the method below:
- Count the number of minor squares of positive or negative deflection in aVF and brand a dot on the aVF axis (see Figure five) moving a mm for each small square counted (e.m. x mm up for negative and ten mm down for positive deflections).
- Count the number of small squares of positive or negative deflection in atomic number 82 1 and brand a dot on the atomic number 82 ane axis moving a mm from the centre of the chart for each small foursquare counted (e.chiliad. ten mm correct for negative and x mm left for positive deflections).
- Depict a horizontal line through your lead 1 dot and a vertical line through your aVF dot and so describe a line from this intersection back through 0 and this volition requite you lot the accurate axis.

Figure 5. The axis of the middle – a useful diagram for assessing the cardiac centrality using the method higher up.
Causes of axis deviation
| Left centrality deviation | Right axis departure |
|
|
6. P-moving ridge and PR interval
- Can you see a p-wave? If the rhythm is atrial fibrillation, atrial palpitate or a junctional tachycardia you may not be able to.
- At this indicate yous can also assess whether each p moving ridge is associated with a QRS complex. P-waves non in clan with QRS complexes point complete heart block.
- Assess p-wave morphology
- In some cases there can be a notched (or bifid) p-wave known as "p mitrale", indicative of left atrial hypertrophy which may be caused past mitral stenosis. There may be tall peaked p-waves. This is called "p-pulmonale" and is indicative of correct atrial hypertrophy often secondary to tricuspid stenosis or pulmonary hypertension.
- A like picture tin can be seen in hypokalaemia (known as "pseudo p-pulmonale").
- The PR interval may be prolonged in first degree centre cake (described in more item subsequently).
- The PR interval may be shortened when there is rapid conduction via an accessory pathway, for example in Wolff Parkinson White syndrome.
- PR depression may be seen in pericarditis.
7. Assessing Q-wave and QRS complex
- Q-wave
- A q-wave is an initial downward deflection in the QRS complex. These are normal in left-sided chest leads (V5, vi, lead I, aVL) every bit they stand for septal depolarization from left to right. This is as long as they are <0.04secs long (i small square) and <2mm deep.
- If q-waves are larger than this or present in other leads they are pathological.
- QRS circuitous
- Width
- The QRS complex normally lasts for < 0.12 secs (3 pocket-sized squares).
- Causes of a wide QRS:
- Bundle branch blocks (LBBB or RBBB)
- Hyperkalaemia
- Paced rhythm
- Ventricular pre-excitation (e.g. Wolf Parkinson White)
- Ventricular rhythm
- Tricyclic antidepressant (TCA) poisoning
- Shape and tiptop
- The QRS may be pocket-size (or depression voltage) in pericardial effusion, loftier BMI, emphysema, cardiomyopathy and cardiac amyloid.
- The QRS is tall in left ventricular hypertrophy (LVH)
- The criteria suggestive of LVH on the ECG is if the height of the R wave in V6 + the depth of the S wave in V1. If this value is >35mm this is suggestive of LVH.
- The QRS tin besides be tall in young, fit people (especially if thin).
- Width
viii. ST segment
- The ST segment can be normal, elevated or depressed. To exist pregnant the S-T segment must exist depressed or elevated by 1 or more than millimeters in 2 consecutive limb leads or 2 or more millimeters in 2 consecutive chest leads. Look out for reciprocal changes.
- ST peak indicates infarction.
- ST depression is usually due to ischaemia.
- ST segment depression may too be seen in digoxin toxicity. Hither the ST depression will be downsloping (sometimes known equally the "reverse tick" sign).
NB: High-takeoff
- A mimic of ST tiptop is high-takeoff. High-takeoff is besides known as benign early repolarization.
- Loftier-takeoff is where there is widespread concave ST superlative, often with a slurring of the j-signal (start of the ST segment). It is almost prominent in leads V2-5, is normally in young health people and is benign.
- The best ways to differentiate it from myocardial infarction are:
- The ST segments are concave; they are most prominent in V2-v; they have a slurred offset (j-betoken); the ST peak is usually minimal compared to the amplitude of the t-moving ridge; there are no reciprocal changes; the ST segments practice not change over time.
9. QT interval
- The QT interval is the time between the start of the q-wave and the end of the t-wave.
- The QT interval is corrected for middle rate giving the QTc.
- As a quick check, if the t-waves occur over half way betwixt the QRS complexes the QTc may be lengthened
- Non an accurate method merely very quick!
- As a quick check, if the t-waves occur over half way betwixt the QRS complexes the QTc may be lengthened
- A long QTc interval (known as "long QT") is particularly of import to identify in patients with a history of collapse or transient loss of consciousness.
Causes of long QT:
| Drugs | Metabolic | Familial | Other |
|
|
|
|
10. T-wave
The t-moving ridge can exist flattened or inverted for a number of reasons:
- Normal variant
- Normally inverted in aVR and V1 and often in V2 and V3 in people of afro-Caribbean descent.
- Ischaemia
- Ventricular hypertrophy (strain blueprint) ordinarily in lateral leads
- LBBB (t-wave inversion in the anterolateral leads)
- Digoxin
- Hypokalaemia (can cause flattened t-waves)
N.B. Hyperkalaemia causes peaked T waves. The classic changes in hyperkalaemia are:
- Small p-wave
- Tall, tented (peaked) t-wave
- Wide QRS
- Widening of the QRS indicates severe cardiac toxicity
Summary
Post-obit steps 1-x in a higher place give the ideal system for interpreting an ECG. If you work through these steps you will be unlikely to miss anything significant.
Click here for the next section: how to identify bundle branch blocks
…and click here for medical student OSCE and PACES exam questions about ECGs
wilsondientooltaid.blogspot.com
Source: https://oxfordmedicaleducation.com/ecgs/ecg-interpretation/

0 Response to "Reading Ekgs Life in the Fast Lane"
Post a Comment